There is no knowing how many babies Fran Hobson has helped bring into the world, having worked as a midwife across the UK for three decades.
From learning the customs and traditions of different cultures, to transforming the choices available for women at a small rural hospital in the north-east, it’s fair to say that Fran has seen it all.
Fathers pacing the floor, and even an audience of cows after a woman was unable to make it to the labour ward in time, Fran has witnessed pre and post-natal care transform over the course of her career.
But regardless of the steady march of science, Fran believes one principle has always remained the same. Mother and baby are at the heart of everything, with family mere bystanders when it comes to the final push.
As International Women’s Day approaches, Your Life has looked back at the deeply intimate world of childbirth, to see what has changed for women over the passing years.
Having children is no longer seen as the pinnacle, with the cost of childcare and preference for career and travel cited as reasons for eschewing parenthood.
There is no denying that the issues which women faced both in the past and present can be magnified upon entering a maternity unit though.
Epidurals were not on offer until the Seventies, and prior to that pain relief came in the form of gas and air, pethidine or a get-on-with-it attitude.
Greater gender equality has contributed towards an increase in female consultants, body autonomy, access to contraception and a vast improvement in education.
Long gone are the days when a woman would fall pregnant repeatedly because contraception was not readily available – or she was forced to slip a curtain ring over her ring finger in a bid to not be socially ostracised as an unmarried mother.
From home births swapped for hospital, certain elements may even be coming full circle with home deliveries rising in popularity once more.
We spoke to retired midwives, both to celebrate the profession and question if equality has been achieved at the moment when women may need it the most.
Fran Hobson, retired midwife
There are few moments in life when a woman may feel as vulnerable, or be required to summon up such an indescribable amount of strength both mentally and physically – regardless of whether the birth is viewed as “normal” or occurs via C-section.
Fran Hobson may not have kept a record of how many babies she delivered, but she believes each and every birth she attended was a complete privilege.
A mother and grandmother, Fran gave up midwifery in 2004 in order to become a health visitor, before retiring altogether in 2014 following ill health due to a car accident.
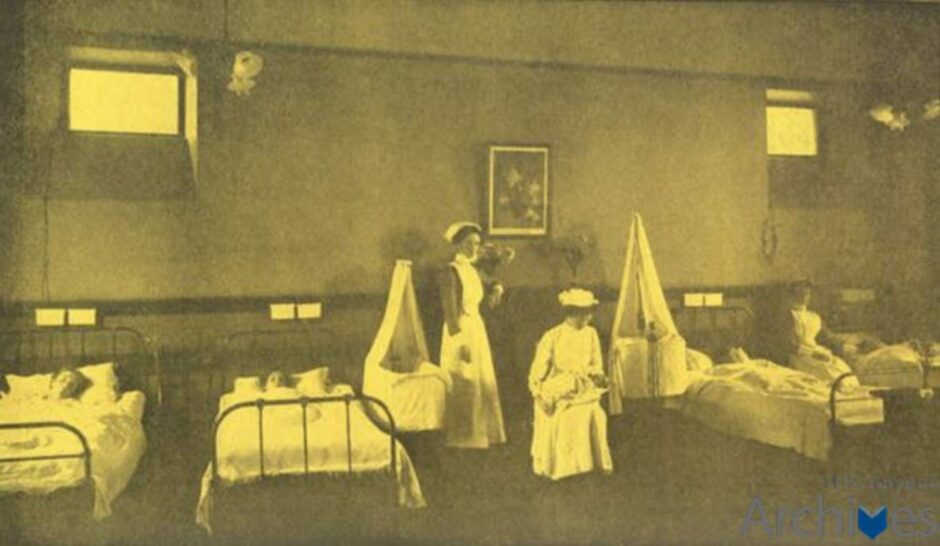
She spent the latter part of her career within the maternity unit of Chalmers Hospital in Banff, known locally as Banff Hilton due to the high standard of care given to expectant mothers.
“I did my general training in Aberdeen between 1971 and 1974,” said Fran, who now lives near Turriff.
“In those days you couldn’t do direct entry to midwifery. You had to do general nursing first followed by a conversion course.
“You also weren’t allowed to do midwifery in Aberdeen if you had already done your general training there, you had to go somewhere else.
“I headed for Peterborough; it was a huge overspill town for London so there was a massive amount of deliveries.
“It was such a varied experience.”
Fran found herself immersed in the Bangladeshi community, with many labouring mothers unable to speak English.
“It was a completely different world, as quite a lot of Bangladeshi women wouldn’t let men anywhere near them,” she said.
“These included male doctors, and at the time there was a huge amount of male doctors.”
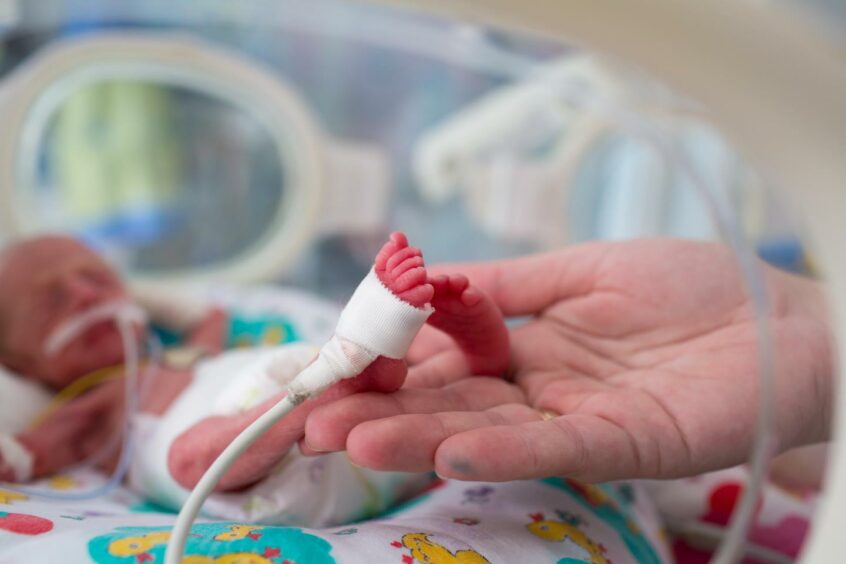
Fran spent the first four years of her career caring for premature babies in the neonatal unit, where she saw science come on leaps and bounds.
“It was at the time when we started to try and push the ability to keep babies alive at earlier gestations,” said Fran.
“Prior to that, the baby would simply be kept warm and comfortable. If they survived, they survived. And if they didn’t, they didn’t.
One of the last straws for me was when a baby died whilst I was on duty, and the baby had been due to go home that same day.”
Fran went on to have two children of her own, before commencing work in Banff in 1984. The maternity unit became midwife led in 1999, a change which Fran believes benefited women greatly.
“It made such a massive difference because we changed the philosophy of how we looked after women,” said Fran.
“We looked at normal labour and how women coped with it. Anxiety can make you produce hormones which fight against labour.
“But if you keep things calm, dim the lighting when possible, add music, it made such a huge difference.
“I did a number of deliveries in an ambulance where a woman had to be transferred to Aberdeen. Of course there was no Western Peripheral Route, so it took over an hour to get to the hospital.
“It was Sod’s Law that the woman would deliver on the way.
“One time I was bleeped by a colleague because a woman was labouring in her car, and it turned out that I was really quite close.
“I found her on a little side road. She was in the front seat which was difficult because the gear stick got in the way.
The baby was born and I’ll never forget, as when I turned round there was a row of about 15 cows looking at us over the fence.
“I’ve had some amount of audiences in my time, but never cows.”
With a better understanding of how women labour, the default position for giving birth is no longer tucked up in bed with as little fuss as possible.
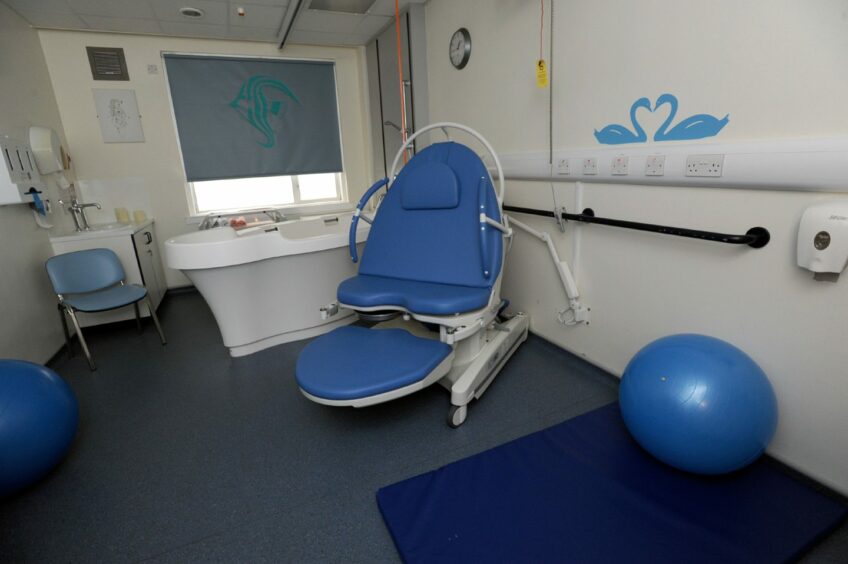
Many midwife led units now offer a range of equipment, from specialist birthing chairs to water births.
Mums to be are also more likely to voice their wishes, from pain relief options to requesting immediate skin to skin.
“I think society has changed greatly,” said Fran.
In my parents’ day, and even when I first started, women didn’t really have a say. They were told what was going to happen.
“This wasn’t just in midwifery but in general. I think if women know how their care is going to go, it is much more acceptable to them.
“I was a midwifery sister at a maternity unit in York in 1980.
“I worked with an old midwife, she used to slap women on the leg and tell them not to make such a fuss because labour couldn’t possibly be that painful.”
“After I had my first son I was very tempted to say to her, well actually it is that painful.
“I don’t ever recall doing a delivery where I didn’t feel it was an absolute privilege to be with that person, to help them and support them.”
Tracy Miller, semi-retired midwife
Once a midwife, always a midwife.
Tracy Miller may have officially retired in 2020, but she stills returns to the ward to do bank shifts.
She can still remember when midwives and indeed all nursing staff were required to wear a different uniform from the tunic and blue trousers which we have grown so familiar with.
Although the get-up was not quite Call The Midwife style, it wasn’t far off.
“Midwifery wasn’t something I originally wanted to do,” said Tracy, who lives in Stonehaven.
“I did nursing first and went on to work in the operating theatres at ARI.
“I had a bit of a disagreement with a surgeon though, and then it wasn’t so fun anymore.
“I decided to give midwifery a bash, it was an 18-month-long course. I qualified and ended up working as a midwife for 30 years.
“Beyond the 40 babies I delivered in order to qualify, I didn’t keep track and I wish I had.”
Tracy estimates that she went on to care for thousands of babies, and became a community midwife in 1996.
The role saw her become even deeper entwined with local women, and she also witnessed a rising popularity in home births.
“Living and working in the community means I am known as the midwife here,” said Tracy.
“Home births are coming full circle now, they have become more publicised.
“There used to be one home birth every two years when I started working in the community.
“In our team we now see 10 to 15 home births each year.”
That’s not the only change, and the blue tunic which Tracy wears when on shift was once a far more formal affair.
“As a student nurse, you wore a white dress with pale pink epaulettes, a paper hat, white shoes and tights.
“The tights were horrible because they made your feet stink from sweating. The hospital laundered your uniform for you, and you always had to look well presented.
“When you qualified, the epaulettes changed to bright pink. That was such a proud moment, but also scary.
“I think women’s requests are more likely to be listened to these days, although we as midwifes of all people want the woman to have a good experience.
“We get women through labour with a bit of coaching, which empowers them.
“Midwifery is still female dominated.
“There used to be only one or two female consultants. Now the majority are female.
“Like any profession, there are good and bad characters.
“Women together can achieve great things though.”
Tracy had her first child during her training, and can recall the senior tutor warning students to make sure they had contraception in place.
“The message was that we shouldn’t get pregnant when doing the course, I didn’t listen to that,” she said.
“I only took six weeks off, I was studying and sitting exams with a newborn.”
Tracy went on to have three children in total, who were all delivered by colleagues via C-section.
My first child was what we call face presentation. If this had been 200 years ago, we would not have survived.
“I went to Nepal for four weeks with The Royal College of Midwives, and it makes you realise how lucky we are.
“The maternal death rate there is much higher, you realise how good the NHS is in comparison.”
Tracy retired in 2020 when, coupled with the menopause, she started to find on-call hard going.
“Computerised notes also came in,” she said.
I am of an era where we weren’t brought up with computers. You aren’t looking at a woman, at her face or asking how she is.
“My colleagues still pulled out all the stops for my retirement, I would have had a big party were it not for Covid.
“You just look back and think wow, I have impacted so many people’s lives.
“I still look at couples and think wow, you made that.
“The miracle of birth has never stopped amazing me.”