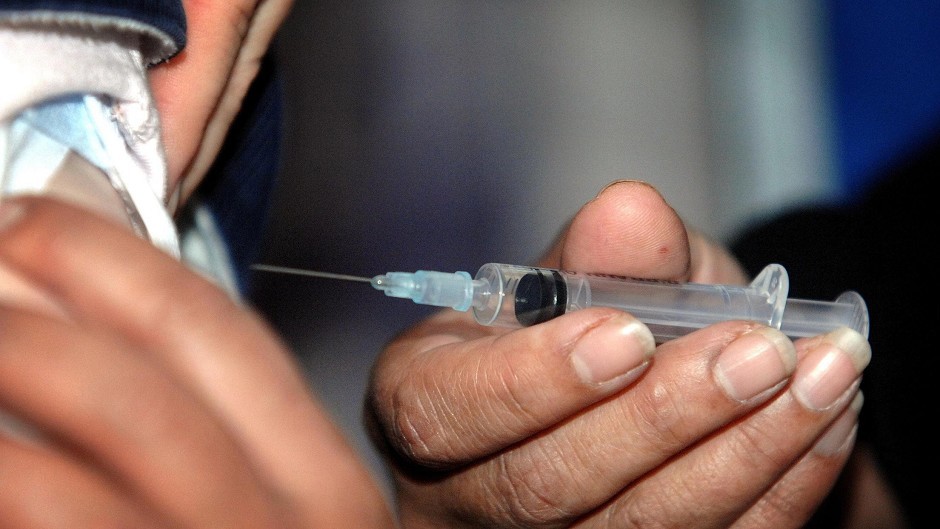
“What did that nasty Dr Mack just do to you?”
I must admit I was a bit put out by this comment from a mother to her young son as she consoled him after I gave him a routine vaccination, many years ago. I didn’t go into medicine to hurt people, but it is part of the job that sometimes I must stick needles, or even scalpels, into my patients, over and above the occasional undignified examination.
Mind you, I do prefer to be at the blunt end of any needle and I am sure this mother was just saying out loud what we are all thinking as we sit there anticipating that sharp point heading for our arm.
I hope that young child has grown up to be a healthy and happy young man, protected from what were common illnesses when I grew up. I have vague memories of the misery of mumps and measles as a child, but I now fear I would be poorly prepared to diagnose these illnesses in my own patients. In the thirty five years since I started at medical school I have never seen a case of measles and what truly scares me is that the tide has turned and we face an increased likelihood of seeing its return.
Vaccinations against infection have transformed our lives. In the past, children would have routinely died from Tetanus, Measles, Diphtheria, Meningitis and Whooping Cough, with many more made seriously ill or left disabled. This is easy to forget as these illnesses fade into our medical footnotes and memories. As the incidence of these illnesses has fallen to the negligible it feels like our individual need for protection has ended, but this is only the case for illnesses such as smallpox, which has been declared eradicated. For all the others we are now protected by “herd immunity”, meaning if everyone around us has been immunised, we are safe. Increasingly, we are having the jags to protect the population as much as ourselves.
Last Saturday morning my practice went into all-out vaccination mode. Three nurses, a healthcare assistant and me, supported by a squad of staff, fortified by bacon rolls, set to with flu vaccines upon 350 of our patients, at three-minute intervals. Invitations had gone out to everyone over 65 and those younger who are carers or living with long-term illness. One-off shingles and pneumonia vaccines were added for those reaching the appropriate age milestone or missed from previous invites.
I am pleased to say it all went smoothly. The vaccines had all been ordered and delivered in their temperature-controlled boxes and patients were surprised to find lots of parking spaces with fewer staff in the buildings. They were efficiently directed to a consulting room where the five of us rotated round giving the jags and recording each in the patient’s notes.
There is a different satisfaction from this sort of work; patients do not generally thank you for the illnesses they don’t get but they are grateful for the protection and to be able to receive it in a calm and efficient manner.
Some are wary, having heard the social media scares. It is not surprising that this happens. A mass treatment that involves injecting factory-modified proteins from the infections we are trying to prevent is ripe for mistrust. These patients need reassurance from health professionals from their own health centre where they have reason to trust us.
For vaccination to work it is crucial to cover as many as possible of the population. It is only then that we can disrupt the spread of infection and prevent epidemics. These invitations to clinics are essential but are not enough on their own. There will be many who do not respond. Some will have their own reasons, but for some of the most vulnerable members of society, barely managing from day to day, making time for the flu jag will have low priority. But fortunately, these people are also more likely to see us for ongoing care of other matters. Our electronic patient record will flag these missing vaccinations and from there it is an easy matter to head for the fridge to find and administer the missing jag.
But this system is under threat. A new GP contract that is being implemented will see a separate organisation take responsibility for vaccines. It is estimated that it will be three or four times more expensive than GP practice administration and the staff will not have access to the GP record to support them. I fear that coverage will also drop as we will no longer be in a position to give those opportunistic jags to the frail and vulnerable and the need for an efficient system will mean fewer options or perhaps a longer distance to travel to a vaccination clinic. Why this was negotiated I do not understand; more than eighty percent of GPs in NHS Highland stated, when surveyed, that they wished to continue to deliver this service if it was appropriately funded.
Miles Mack
October 2019
Dr Miles Mack is a GP in the Highlands and the former chair of the Royal College of General Practitioners Scotland