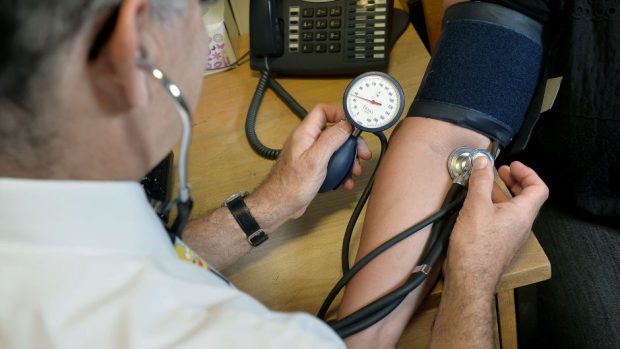
For some reason I started shaking uncontrollably on my hospital bed as I was being examined.
It was odd as I felt perfectly calm and relaxed otherwise. It dawned me on that I was not the problem. The bed appeared to be shaking.
But then my eyes came to rest on pair of hands which were gripping the bed – and they were not my own. They belonged to a medical student and it was he who was shaking as though he had just stepped out of a freezing outdoor plunge pool in the Arctic.
It was not the most promising bedside manner, but I must point out that we were thrown together in a particularly fraught situation and he was gripped by a bad case of stage fright.
It might sound a bit peculiar, but I was one of several volunteer patients roped in for an important assessment in medical school where students were role-playing under the eagle eyes of senior tutors. Students were briefed about our imaginary “symptoms” before having to demonstrate how to carry out detailed and technically correct examinations. It was a big challenge to practice on real people and occasionally rather unnerving for “patients”, too.
Now and again a student doc would go off-brief and start examining me for real – pointing to actual potential afflictions around my body which alarmed them. They alarmed me even more.
After these inquisitive types departed one of the official invigilators (a senior medic in their own right) would grab a stethoscope and examine me hastily before the next one came in – and assure me I was not about to have a heart attack after all. But it demonstrated to me that some intuitive students were already displaying a natural instinctive approach to look beyond the obvious. This could save lives later.
I have to confess that nerves and fear of the unknown also dogged my early days as a student journalist until I started banking some valuable front line experience. The shaking student was taking his first faltering steps to what might have been a great career; what concerns the NHS today are the final steps medical students take when choosing a speciality – as we cry out for more GPs.
Dr Linzi Lumsden is a GP partner in a large Aberdeen practice, and a senior clinical lecturer in GP and community medicine at Aberdeen University medical school for students in years one to three. She would like to see more of them become GPs in an era when shortages of family doctors are being exacerbated by rising retirements, practice closures and patient lists. Health boards in Grampian and Highlands throw the net wide to find experienced GPs, but their own medical students are also part of the solution. It’s like top teams bringing their own home-grown talent through.
So why do many medical students find GP practice a turn off? Is it not glamorous enough for them? Perhaps they have overdosed on too many film and TV medical dramas, or “24 hours in A&E”?
Dr Lumsden, a GP for six years, met me to discuss the problem amid the chatter of medical students having lunch a few feet away – the very people who have these huge career choices to make during a study and training period which can last at least 10 years.
“Medical schools everywhere are not getting enough students to become GPs,” she told me. “Negativity towards GP practice can develop during their studies and training, and the views of some peers and colleagues might drive this along. It creates a perception of a divide between GPs and the hospital side of things.
“Sometimes students have perceptions that the GP sector has lower status.”
Myths are often dispelled by meeting and working with GPs, which is built into medical school training. Third-year Aberdeen student Caitlin Stewart, 26, from East Kilbride, agrees with that.
“We visited a GP’s house where we had breakfast. We saw the lifestyle along with the practice, community hospital and mountain rescue,” she told me. “The highlight was speaking with actual GP trainees about their work at a speed-dating style event. I was impressed with the whole GP experience.”
I also came across an Aberdeenshire doctor blogging about his switch into general practice at a late stage of training instead of becoming a renal specialist. He described his previous misconceptions about “boring” or “too simple” GP work – now blown away by his newfound calling in community medicine.
Dr Lumsden said, “The great thing about GP practice is that you don’t know what will come through the door. We are like NHS gatekeepers, filtering people through. GP practice and hospital casualty are similar in these respects.”
This is where intuition based on experience kicks in. “You have to be like a detective at times. Someone might come in with seven things wrong with them, but it’s the last one which sets alarm bells ringing,” she added.
My earliest GP memories are as a kicking and screaming three year-old when our family doctor sewed my hand back together after a horrible gash caused by falling on broken glass. Decades later my GP decided the time was right for me to visit a consultant. Hospital tests showed I had prostate cancer, but it was caught early.
What would have happened to me without these decisive interventions by GPs on the front line of medicine?
David Knight is the long-serving former deputy editor of the Press and Journal