It sounded like I was being told I had months to live, but in reality the GP had probably just saved my life.
When I was diagnosed with genetic haemochromatosis, I got a phone call asking me to make an appointment with my doctor to discuss my blood test results, was told the news and then immediately offered counselling.
I was 19, had just started university in Edinburgh and was full of boundless energy. The last thing I felt was ill.
The reality was my body was poisoning itself with iron at an extraordinary rate that shocked the consultants I was referred to. My iron levels were 2,500. Depending on who you talk to, normal is anywhere from 20 to 200.
Within weeks, I had a hole punched in my liver to check for damage, and I was at the hospital every week for just over a year to have a pint of blood taken out.
To put that in context – in general, blood donors aren’t allowed to give blood more than once every 12 weeks to ensure they have ample iron. I needed it drained out of me, and fast.
Although it kills, haemochromatosis is actually incredibly easy to manage – but only once you’re diagnosed through testing.
Hard to say, easy to manage, tragic to ignore
When I was diagnosed, I declined the counselling. I was a teenager; I felt fine. What did I need to talk about?
Huntington’s disease runs in my family. I know only too well the consequences incurable genetic diseases can have, but I was told there was treatment for haemochromatosis and I would be fine. No problem.
It’s taken me a long time to fully appreciate the situation I was in. My iron levels when I was diagnosed were more than 20 times higher than what is considered healthy. That was 18 years ago; I’m not good enough at maths to know how high they would be now.
There is undoubtedly a gap in knowledge when diagnosing #haemochromatosis, which I think everyone in my family experienced.
Once diagnosed, after a lot of convincing my GP I could actually have it, my treatment from multiple NHS boards has, in the round, been good #ironoverload https://t.co/XpRNw8uIAt
— David Mackay (@DaveFeatures) October 12, 2023
In my job as a news reporter, I speak to all kinds of people from all different walks of life; it’s the reason I enjoy what I do.
One day, I was chatting to a regular contact who told me she had been very distracted from whatever it was I was calling her about because her husband had recently died. I naturally offered her my condolences, and she said he had been unwell for some time due to haemochromatosis.
My heart stopped. Until that moment, I had only met people like me in waiting rooms or hospital wards who were getting treatment and looked fine.
I was told there could be fatal consequences, but I never considered that a realistic possibility. In just a few seconds all the dots joined in my head and I realised how lucky I had been.
How do you know if you have haemochromatosis?
Do you feel tired a lot? Do you have various aches and pains in your joints? Do you find yourself catching colds or other bugs often?
I’m pretty sure all of us will say yes to at least one of those questions because they’re mostly all just part of life and nothing to worry about.
However, for those with haemochromatosis, these symptoms can be a sign that their iron levels are too high, and they should ask for blood or genetic testing.
I’m due to give blood next month and can tell my levels are higher than they should be. I’m tired and get headaches often. Nothing major, really.
My mum was in her 40s at the time, and I’m grateful her GP in Inverbervie speculated something bigger was going on and tested her
Left unchecked, though, your body begins to kill off cells in order to create room to store the excess iron. Cancer, arthritis, liver cirrhosis and diabetes are all common consequences.
Around the time I was diagnosed, unbeknown to me, my mum was making repeated trips to the GP for various, seemingly unconnected worries. She was in her 40s at the time, and I’m grateful her GP in Inverbervie speculated something bigger was going on and tested her.
Hearing about the death of Miranda McHardy in Banchory was difficult. It’s hard not to imagine that might have been me or my mum.
Distributing haemochromatosis testing kits is an incredible way for her family to honour her memory. I am certain lives will be saved as a result.
How a haemochromatosis diagnosis can also help you save lives
When you’re diagnosed with haemochromatosis, the first thing a doctor will do is tell you to eliminate iron from your diet as much as possible, and to stop drinking alcohol.
Fortunately, I was caught early enough not to have any permanent damage, so still enjoy steak and beer in moderation. I stay clear of orange juice, though: vitamin C can increase the rate at which your body absorbs iron.
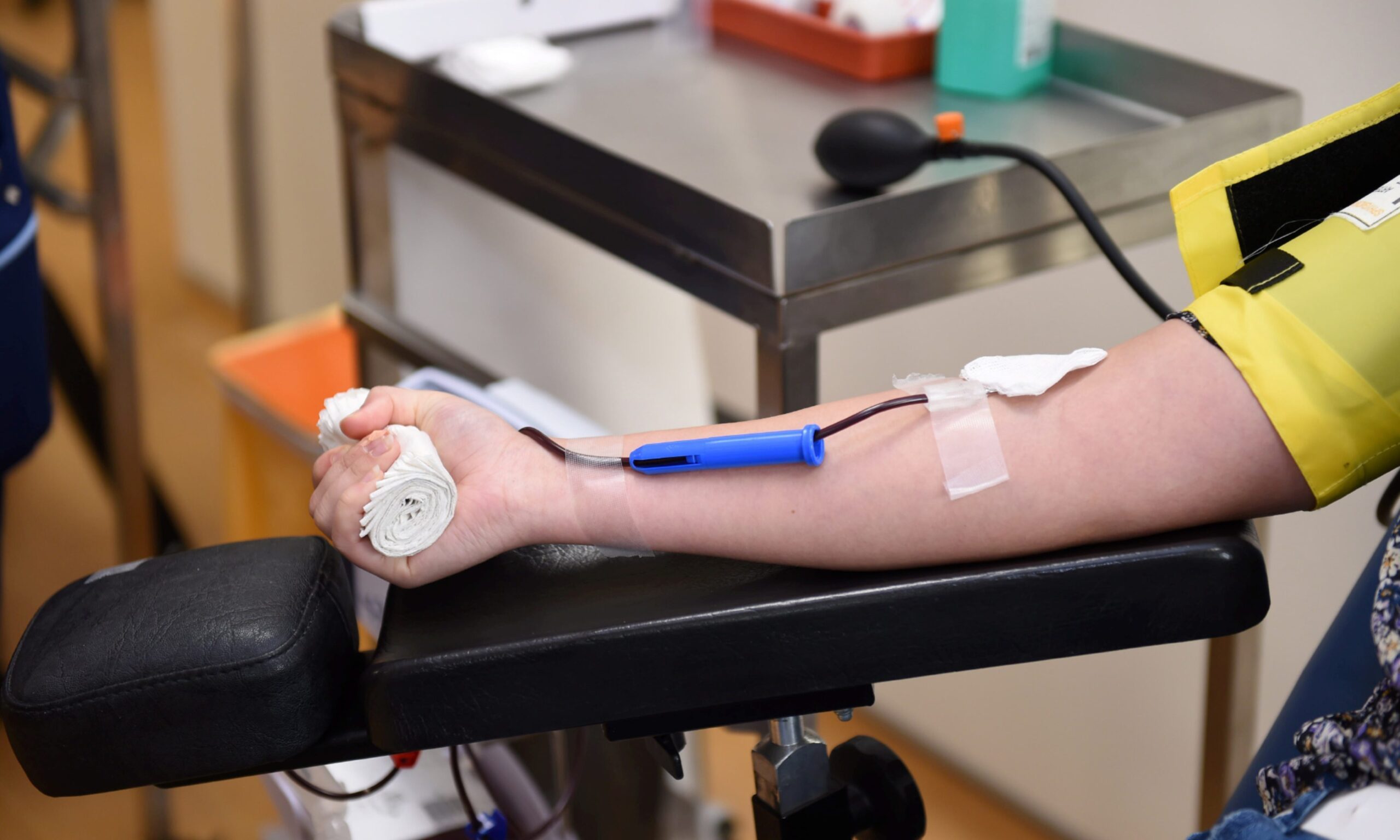
The only way to reduce your iron levels is to have blood removed, which forces your body to use the excess iron to replace what has been lost. This is initially done at hospitals or GP practices, depending on where you live, and, sadly, that blood gets incinerated.
Once your levels become normal, though, you can be approved for visits to a blood donor centre, which has the double benefit of helping your own health while also potentially saving the lives of others.
When I know my levels are high, I’m always looking for when and where the nearest donor session to me is. In the last year or so I’ve donated in Elgin, Lossiemouth, Forres, Aberdeen and Inverness.
It’s a good arrangement, but improvements can still be made. Haemochromatosis patients can donate more often in England and Wales, a rule that I know is being examined in Scotland.
Visiting the blood bank may be a constant reminder of my diagnosis – and I think about it a lot when I’m there lying on the bed, admiring the wooden ceiling at Elgin Town Hall – but it’s something we should all do anyway.
Ultimately, I know I’m going to be fine, and there are far worse genetic diseases out there. I got off lightly – make sure you’re the same by getting tested.
David Mackay is a news journalist with The Press and Journal in Elgin. He is always counting the days to his next blood bank visit
25,000 households to be tested for ‘Celtic Curse’ after death of Banchory woman










Conversation